In this webinar, as the fifth part of the Science of Aging Webinar Series, Dr. Dudley Lamming discusses his research on how diets can affect metabolic health and longevity.
Highlights
- The role of fasting in calorie-restricted diets
- The effects of low protein versus high protein diets on weight, fat mass, and fasting blood sugar
- The metabolic effects of the branched-chain amino acids
- Reducing consumption of branched-chain amino acids to promote health and longevity
Webinar Summary
Dr. Lamming begins the webinar with an explanation of how mouse models in the lab are used to study nutrition and metabolism; as omnivores with an abundance of choice, studying these topics in humans is much more complex.
“We’ve known for a number of years . . . that restricting caloric intake is a very effective way of extending health and lifespan in numerous species.”
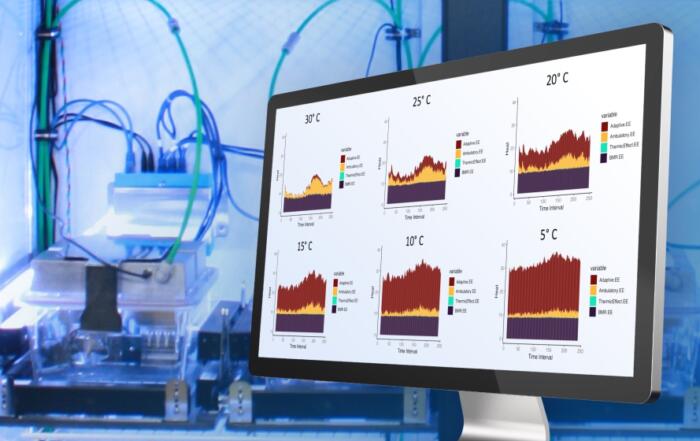
He proceeds to explain the role of fasting in calorie-restrictive (CR) diets as well as the importance of protein, particularly branched-chain amino acids. Time-restricted eating has been shown to have significant effects and improve metabolic health; one study showed that meal feeding, where calories are not restricted but animals are inadvertently fasted, had a positive effect on survival. Dr. Lamming’s research thus sought to investigate whether the benefits of calorie-restriction (in terms of lifespan and metabolic health) are due to calorie-restriction, imposed fasting, or both. The first section of this webinar discusses the findings of these experiments, in which mice were fed distinct diets varying in time-restriction and calorie-restriction. The results revealed less weight gain and/or weight loss overall compared to the control, but different resulting effects for each diet. In summary, fasting and decreased energy expenditure both contribute to the metabolic and molecular effects of a CR diet; fasting alone proved sufficient to produce positive effects on both metabolism and transcriptional profiles, and decreasing energy intake without a fasting period did not promote robustness nor increase lifespan.
The next part of the webinar focuses on diet and the three main macronutrient categories: protein, fat, and carbohydrate. Historically, protein was thought to be beneficial, but recent research revealed that mice fed low protein diets had the longest life span. In fact, many long-term studies have shown low-protein diets are associated with improved health in the general population. To determine whether this was translatable to humans, a clinical study was conducted. Dr. Lamming explains that the results indicate a protein-restricted diet reduced weight, fat mass, and fasting blood sugar; however, calorie consumption was actually higher in this group. Dr. Lamming’s group sought to investigate whether these metabolic effects can be observed in a mouse model, and found that mice fed low protein diets responded similarly to humans: weight gain and fasting blood glucose were reduced despite increased food intake accompanied by greater energy expenditure.
Dr. Lamming continues the webinar with a focus on amino acids (AAs), specifically the branched-chain amino acids (BCAAs) leucine, isoleucine, and valine.
“BCAAs have been known to be associated with insulin resistance for a long time.”
His group found that mice fed a low BCAA diet look similar to PR mice: they ate more but gained less weight. Additionally, restricting both BCAAs and all AAs improved glucose tolerance, and in particular, dietary isoleucine and valine are potent regulators of glucose tolerance. Further, restriction of dietary leucine is necessary to realize the benefits of a low AA diet. Dr. Lamming proceeds to describe how FGF21, an insulin-sensitizing hormone produced in response to fasting, plays an important role in energy expenditure in a low isoleucine diet but does not mediate improvement of glucose tolerance.
“Overall, it looks like FGF21 accounts for half or even a little more of the increased energy expenditure that’s mediated by a low isoleucine diet.”
He continues that simply restricting either isoleucine or valine dramatically decreases weight and fat mass, equivalent to the effects observed when following a low BCAA diet. The question of whether this would also be true in humans led to his ongoing study investigating a BCAA-restricted diet in overweight, pre-diabetic humans. Epidemiological work done in parallel revealed that relatively small increases of isoleucine proportion of total protein was associated with increased BMI.
“Overall, we think people may want to rethink what they eat . . . IF humans respond to dietary protein and BCAAs the same way that mice do . . . and we may also want to rethink when we eat . . . so if humans respond to fasting in a way similar to mice, the fasting component may be very important to include.”
The webinar concludes with a note that early consumption of a low BCAA diet extended lifespan in males but not females and a brief highlight on the sex-specific impact of this diet on the skeletal muscle transcriptome.
Resources
Q&A
- What time of the day did you conduct the GTT (Glucose Tolerance Test) and ITT (Insulin Tolerance Test)?
- How do you stimulate amino acid oxidation?
- Why didn’t the calorie-restricted group of mice that were fed once per day enter torpor?
- Does classic calorie-restriction improve cognition in the aging brain and reduce incidence of Alzheimer’s disease?
- Have you looked at markers of oxidative stress in calorie-restricted or fasted mice, and if so, what role do changes in reactive oxygen species have on glucose tolerance or insulin sensitivity?
- With a low protein diet, were there any changes noted in autophagy in muscle islets or hepatocytes?
- Have you tested the influence of temperature on the metabolic effects of isoleucine?
- How has this research changed your own (Dr. Lamming’s) eating patterns?
- How is the effect of isoleucine on decreased fat in body composition mediated?
- Why did you decide to feed the mice at the beginning of the light phase when they normally eat during the dark phase?
- How would endurance exercise for glycogen depletion affect the fasting versus ad libitum feeding models?
Presenters
Associate Professor
Medicine
University of Wisconsin-Madison